Blog
Concerned About Fentanyl Use? Symptoms Families May Notice First

Sometimes the first sign is not dramatic. A person may seem unusually sleepy at odd hours, harder to wake, less steady, or less present in conversations that used to feel normal. For families, that can bring a mix of fear, confusion, and second-guessing.
Some fentanyl addiction symptoms can overlap with stress, depression, other substance use, or a medical problem. Still, certain patterns deserve attention, especially when changes in mood, alertness, daily functioning, and physical health begin to cluster together.
Why fentanyl can be hard to recognize early
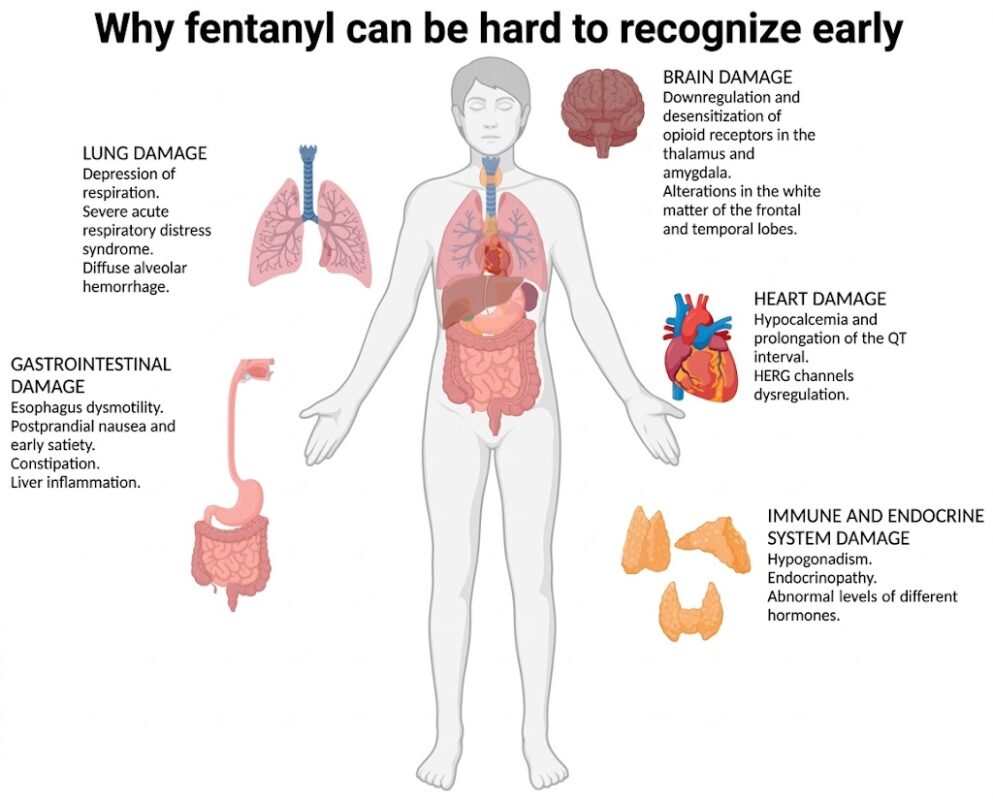
Fentanyl is a very potent synthetic opioid. In real-world settings, people are not always aware they have taken it, especially when it is mixed into other substances. Research on illicitly manufactured fentanyl also shows that exposure, metabolism, and effects can vary, which can make early warning signs less predictable from one person to another.
That uncertainty is part of what makes this so difficult for families. You may notice something is off before you can name exactly what it is.
Early changes families may notice
Early signs often show up as a pattern rather than one single symptom.
A person may seem more drowsy than usual, nod off unexpectedly, or move through the day in a slowed, heavy way. Their speech may sound softer or more slurred. They may become less responsive, miss plans, or seem disconnected from what is happening around them.
Behavior can shift too. Some families notice secrecy, changes in routine, unexplained disappearances, or a sudden need for privacy around money, phones, bags, or time away from home. Irritability can rise, especially when the person is questioned or interrupted.
Physical changes can be easy to dismiss at first. You might see pinpoint pupils, frequent fatigue, nausea, constipation, or a general decline in grooming and appetite. Sleep may become irregular. The person may seem either deeply sedated or restless and uncomfortable between periods of use.
None of these signs proves a fentanyl-related problem on its own.
What matters more is the repeated pattern, the speed of change, and whether daily life is starting to narrow around getting, using, or recovering from a substance.
Symptoms that may suggest dependence is developing

Dependence means the body has adapted to the drug and reacts when it is reduced or stopped. With opioids, that can happen alongside addiction, though they are not exactly the same thing.
Common signs include needing more of the substance to get the same effect, using more often than planned, or feeling unwell when it wears off. A person may say they are taking something just to feel “normal” or to avoid getting sick.
Withdrawal can include body aches, sweating, chills, anxiety, trouble sleeping, nausea, vomiting, diarrhea, restlessness, and intense cravings. Recent reviews suggest fentanyl withdrawal can be especially difficult to manage, and some newer studies note that the presence of other substances such as xylazine or medetomidine may complicate symptoms further. That means the picture is not always simple, and what families see may look more severe or unusual than expected.
Emotional and behavioral warning signs
Addiction often affects more than the body. It can change priorities, relationships, and emotional regulation.
A person may pull away from family, lose interest in usual routines, or seem caught between shame and defensiveness. Some become more isolated. Others cycle between sedation and agitation. Work, parenting, school, or household responsibilities may start to slip.
You may also notice a pattern of promises that do not hold up, not because the person does not care, but because substance use has begun to overpower intention. That distinction matters. It does not erase harm, but it can help families respond with clearer eyes and less blame.
When symptoms may point to overdose instead of ongoing use
This is one area where families should not wait and see.
Warning signs of opioid overdose can include very slow or stopped breathing, a person who cannot be woken up, blue or gray lips or fingernails, limpness, choking sounds, or a very small pupil size with extreme unresponsiveness. Fentanyl is strongly associated with respiratory depression, which means breathing slows enough to become dangerous.
When this kind of change happens, it is a medical emergency.
Why today’s fentanyl picture is more complicated
Street drug supplies can contain fentanyl alone, fentanyl analogs, or fentanyl mixed with other compounds. Some published studies describe growing concern about combinations involving xylazine and, more recently, medetomidine in some areas. These combinations may alter withdrawal, sedation, and overdose patterns.
That does not mean every person will show the same symptoms. It does mean families should be cautious about assuming they know exactly what was taken or what will happen next.
What families can do when they are worried
Start with observation, not accusation. Specific examples usually help more than global statements. Saying “I’ve noticed you’re falling asleep mid-conversation and missing work” is often more grounding than “You’re ruining your life.”
Try to talk during a calmer moment, not during obvious intoxication or a heated argument. Keep the focus on safety, health, and concern. Shame tends to shut conversations down.
It may also help to involve a doctor, addiction specialist, or treatment program rather than trying to sort it out alone. A professional assessment can help distinguish opioid use, withdrawal, overdose risk, and other medical or mental health issues that may look similar.
Treatment is possible, even when things feel messy
People with fentanyl-related opioid use problems can improve with treatment. Care may include medications for opioid use disorder, withdrawal support, behavioral therapy, and ongoing follow-up. Recent clinical writing on buprenorphine induction notes that fentanyl can make treatment planning more complex in some cases, so individualized medical support matters.
Recovery does not always begin with one perfect conversation.
Sometimes it starts with naming what is happening clearly.
Reducing immediate risk, and getting the right clinical support involved.
You do not have to be certain of every detail before taking concern seriously.
A grounded way to think about these signs
Families often look for one unmistakable clue. More often, the clearer picture comes from accumulation: sedation, behavior changes, secrecy, physical symptoms, withdrawal-like illness, and shrinking daily function.
That does not mean every concerning change is fentanyl-related. It does mean a repeated pattern deserves attention, especially with a substance linked to a high overdose risk and an unpredictable illicit supply.
If you or your family are worried, reaching out for a professional evaluation is a reasonable next step.
Safety Disclaimer
If you or someone you love is in crisis, call 911 or go to the nearest emergency room. You can also call or text 988, or chat via 988lifeline.org to reach the Suicide & Crisis Lifeline. Support is free, confidential, and available 24/7.
Research based References
- London, K. S. (2026). Severe fentanyl withdrawal associated with medetomidine adulteration: A multicenter study from Philadelphia, PA. Journal of Addiction Medicine. https://doi.org/10.1097/ADM.0000000000001560
- Sandhu, K. S. (2025). The xylazine-fentanyl nexus: A public health emergency. SAGE Open Medicine. https://doi.org/10.1177/20503121251348068
- Alexander, R. (2025). Withdrawal signs and symptoms among patients positive for fentanyl with and without xylazine. Journal of Addiction Medicine. https://doi.org/10.1097/ADM.0000000000001423
- Skarda, J. L. (2025). Best practices for buprenorphine induction strategies. Journal of Addictions Nursing. https://doi.org/10.1097/JAN.0000000000000670
- Weber, A. N. (2024). Managing opioid withdrawal symptoms during the fentanyl crisis: A review. Substance Abuse and Rehabilitation. https://doi.org/10.2147/SAR.S433358
- Bird, H. E. (2023). Fentanyl absorption, distribution, metabolism, and excretion: Narrative review and clinical significance related to illicitly manufactured fentanyl. Journal of Addiction Medicine. https://doi.org/10.1097/ADM.0000000000001185
- Kiyatkin, E. A. (2019). Respiratory depression and brain hypoxia induced by opioid drugs: Morphine, oxycodone, heroin, and fentanyl. Neuropharmacology. https://doi.org/10.1016/j.neuropharm.2019.02.008
- Pichini, S. (2018). Acute intoxications and fatalities from illicit fentanyl and analogues: An update. Therapeutic Drug Monitoring. https://doi.org/10.1097/FTD.0000000000000465
